Predictive AI for Life-Saving Sepsis Intervention
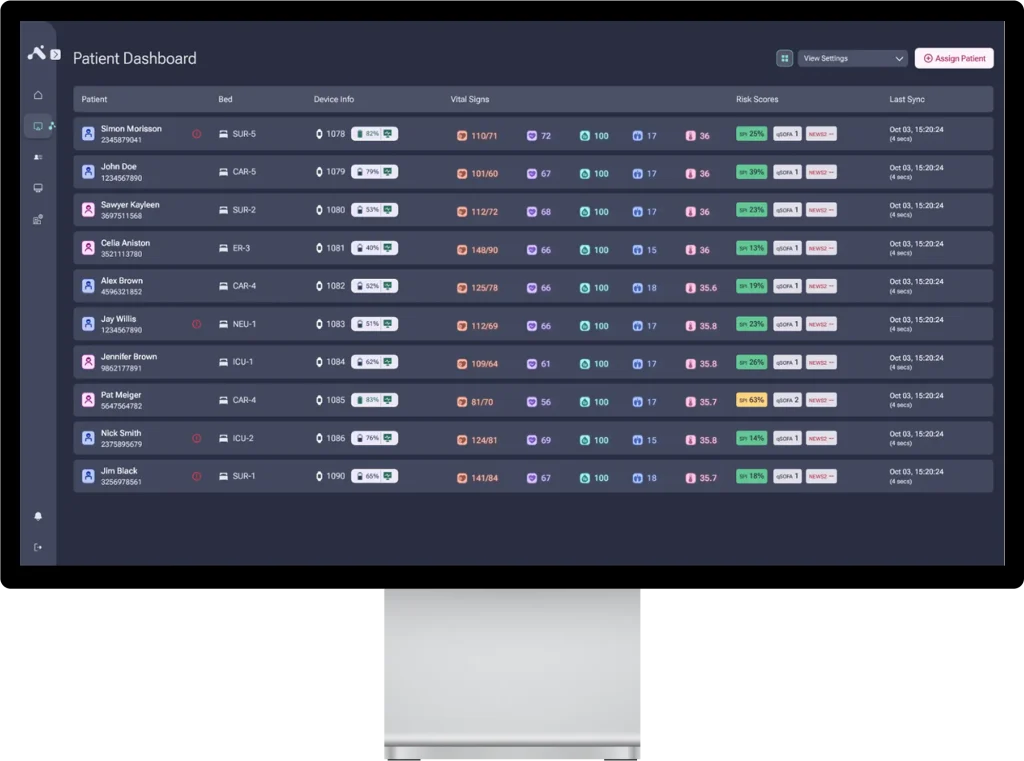
A hospital-grade clinical decision support system integrating the Sepsis Prediction Index (SPI®) to identify sepsis risk up to 48 hours before clinical signs appear, enabling timely, life-saving intervention.
Problem
Every 2.8 seconds, someone dies from sepsis.
Most Cases Are Detected Too Late.
⁶ CDC
System
VIOSync SPI® Overview
The VIOSync Sepsis Prediction Index leverages more than 100 key parameters, drawing insights from 20,000 septic cases used extensively in its development phase.
Data In
Secure and seamless data ingestion from EHRs, ensuring standards- based connectivity (HL7/FHIR)
Digital Patient Twin
Continuous modelling of the patient’s physiology to precisely track and detect the most subtle, early changes in status.
Sepsis Prediction Index (SPI®)
Our explainable AI engine generates a dynamic, validated risk score up to 48h before clinical signs are present.
Actionable Guidance
Delivers clear, site-configurable, protocol-based next steps directly into the clinician’s workflow.
Features
What Clinicians Get with VIOSync SPI®
Real-time risk & trend visualisation
Patient and ward-level visualisation, enabling rapid triage decision-making with trajectories and change-points.
Recommended actions (protocol- aligned)
Sepsis bundle prompts and site-specific pathways surfaced inline.
Transparent rationale panel
Clinician-readable “why this alert” with contributing factors.
Time-aware detection
Recognises when a patient’s state is changing—hours before signs.
Multi-patient triage dashboard
Sort and filter by risk score, new alerts, or overdue actions to prioritise care across the entire ward
In-workflow delivery
EHR launch, patient-list badges, and configurable notifications ensure alerts reach the right clinician immediately
Impact
Clinical & Operational Impact
Early identification of sepsis leads to faster intervention, better outcomes, and significant cost savings.
Reduced In-Hospital Mortality
Shorter Length of Stay (LOS)
Faster diagnosis drives quicker recovery and earlier patient discharge. Studies demonstrate a reduction in patient Length of Stay by up to 32.3% ⁽²⁾, improving bed flow and capacity.
Fewer ICU Transfers
Proactive ward-level care prevents avoidable clinical escalation to critical care. Early intervention with SPI® reduces preventable ICU admissions by an average of 5% ⁽¹⁾.
Operational Cost Savings
Reduced mortality, fewer ICU days, and shorter overall LOS drive material financial impact. Economic models show potential annual savings of up to £2.5M in a mid-size hospital.
Calculator
Quantify the Impact
Estimate your hospital’s potential savings with our interactive ROI Calculator. Adjust your admissions and sepsis caseload to see live projections of reduced ICU stays, shorter ward LOS, fewer readmissions, and total annual cost savings with VIOSync SPI®
- Burdick, H. et al. (2020) BMJ Health Care Informatics
- Adams, R. et al. (2022) Nature Medicine
- Shankar-Hari, M., Harrison, D. A., Rowan, K. M. (2016) Critical Care Medicine
- Hex, N., Retzler, J., Bartlett, C., Arber, M. (2017) The Cost of Sepsis Care in the UK
- Henry, K. E. et al. (2022) Nature Medicine
- Mouncey, P. R. et al. (2015) Health Technology Assessment
Safety
Compliance, Safety and AI Governance
VIOSync SPI® is a Class IIa Medical Device Software developed and operated under an ISO 13485-certified QMS.
Engineering follows IEC 62304 (software life-cycle), usability is evaluated per IEC 62366-1, and risk management is conducted under ISO 14971.
Operations are aligned with GDPR/HIPAA, with DPIA/DTIA available on request.
CE MDR conformity assessment is in progress.


FAQ
Does VIOSync replace clinical judgement or existing screening tools?
No. VIOSync is clinical decision support. It surfaces risk earlier and explains why; clinicians remain the decision-makers and continue using local screening/protocols.
How early is it—and how reliable?
SPI® can flag risk hours to ~48h before overt signs in pilots. Site-specific AUROC/PPV/NPV, timeliness, and alert burden are monitored and reviewed via governance dashboards.
What do clinicians actually see?
A risk score with trend, an explainable “why this alert” panel (key contributors), and protocol-aligned next steps (e.g., SEP-1). Ward and patient views support triage.
Will this increase alert fatigue?
We use priority tiers, throttling, deduplication, and watchlists. Thresholds are tuned with your governance group to a target precision/recall; burden is monitored continuously.
Where does it work—only ICU?
Across wards, post-op, ED, and ICU. Biggest value where deterioration is often missed (general/surgical wards).
Can we tune thresholds and “next-best actions”?
Yes. Both are site-configurable and aligned to your pathways and governance.
What EPRs/EHRs and data do you integrate with?
Standards-based HL7 v2 / FHIR (R4) / IHE for vitals, labs, meds, demographics; optional monitors/wearables. SMART on FHIR launch where supported.
How is it deployed and where is data stored?
Your choice: SaaS (VPC), hybrid bridge, or on-prem (containerised). Data residency options; encryption in transit/at rest, SSO (SAML/OIDC), RBAC, audit trails.
How do you handle bias, drift, and updates?
Subgroup checks (age/sex/comorbidity/site), calibration/drift monitoring, documented mitigations, versioned releases with rollback, and site-specific re-tuning through governance.
Are there financial benefits to Trusts?
Yes. Pilots and economic models indicate fewer ICU transfers, shorter LOS, and reduced complications, driving material net savings. We provide a site-specific ROI model during evaluation (see Evidence for figures).
How do you measure success and ROI?
Joint KPIs: time-to-recognition, timeliness of interventions, LOS, ICU transfers, mortality (where appropriate), alert burden, and economic impact—reviewed with your governance team.
